Neuromuscular diseases
This is a group of hereditary diseases that are transmitted at the genetic level (X-linked, autosomal dominant, autosomal recessive forms, maternally inherited mitochondrial forms). About a third of disease cases are the result of new mutations. Taking into account the structural organization, the following levels of damage to the neuromuscular system are distinguished:
- Primary muscular lesions (muscular dystrophy of Duchenne, Becker, myopathy, myotonia).
- Synaptic lesions (neuromuscular transmission disorders - myasthenia gravis).
- Neuronal lesions (spinal muscular atrophy).
MYOSITIS
Myositis is a group of diseases that manifest as inflammation in muscle tissue. Myositis is caused by various reasons, on which the prognosis of the disease depends. This problem is often encountered by people in professions that involve constantly being in one (often physiologically uncomfortable) position: drivers, musicians (violinists, pianists), athletes (tennis players), programmers, and so on.
Common reasons may be:
1. Infections of a viral or bacterial nature (flu).
2. Autoimmune diseases (rheumatoid arthritis, scleroderma, lupus erythematosus, etc.).
3. The influence of toxic substances (alcoholism, drug addiction).
4. Long-term use of certain medications.
Myositis - symptoms and treatment
The disease is manifested by the appearance of aching or dull pain in the affected tissues. It intensifies with movement or pressure. Muscle weakness is often noted. Redness and swelling of the skin are rare. The most common are cervical and lumbar myositis. They develop due to constant exposure to an uncomfortable position, due to hypothermia, or previous diseases. Often the pain radiates to other areas and intensifies with activity. Treatment is aimed at suppressing inflammation, maintaining a healthy lifestyle, and using dosed physical activity.
SYMPTOMS OF NEUROMUSCULAR DISEASES
The main symptom of neuromuscular diseases is muscle weakness. The clinical picture depends on the affected area (shoulder girdle, hips, pelvis, lower extremities, facial muscles, respiratory muscles). Depending on the form of the disease, muscle weakness and increased fatigue during physical activity develop, muscle atrophy / pseudohypertrophy, fasciculations appear, tendon reflexes are inhibited , gait is disturbed, special motor techniques appear when getting up from a lying or sitting position. Neuromuscular diseases occur in stages. A neurologist will help determine the stage of development of pathological processes using medical diagnostics.
Acquired muscle diseases
Acquired muscle diseases can be of inflammatory, infectious, drug, or toxic origin.
Inflammatory diseases of human muscle - polymyositis, dermatopolymyositis, inclusion body myositis, sarcoid myopathy.
Infectious myositis can be viral, bacterial, parasitic, etc. The main symptoms - muscle weakness and pain - appear acutely. Sometimes they may be accompanied by skin lesions (dermatopolymyositis). A distinctive feature of the course of these diseases is an increase in body temperature.
DIAGNOSTICS
The diagnostic task is to establish the level of damage to the neuromuscular system, establish the cause and determine whether there is a specific treatment.
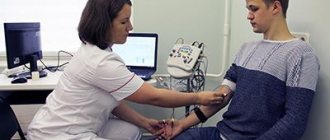
- Electroneuromyography and electromyography. Diagnostic methods help determine primary and secondary myopathy. Also assess the degree of damage to the spinal cord and peripheral nerves.
- Laboratory tests. A clinical and biochemical blood test is required to determine the level of electrolytes, protein, lactate, CPK, ALT, AST, myoglobin and thyroid hormones.
- Muscle biopsy with pathomorphological examination of muscle tissue. The diagnostic results help to establish an accurate diagnosis (Duchenne, Becker muscular dystrophy), which is important for selecting the correct therapy.
- Molecular genetic diagnostics is the most informative diagnostic method, which is prescribed for neuromuscular diseases.
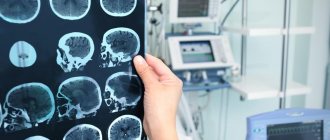
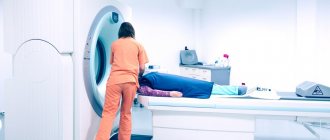
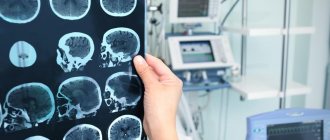
- Magnetic resonance imaging of the brain and cervical spine.
- An electrocardiogram (ECG) evaluates heart rhythm.
- ECHO CG reveals hypertrophic, dilated cardiomyopathy.
TYPES OF MUSCLE DISEASES
Muscle diseases are divided into groups that have a similar occurrence, characteristic manifestations, course and treatment methods.
Diseases include:
- myasthenia gravis – muscle weakness due to autoimmune processes;
- myalgia – pain in muscle tissue due to cell spasm;
- myositis - inflammatory processes that occur against the background of infections, parasites, and other causes);
- Rhabdomyolysis is a serious disease that develops due to the destruction of skeletal muscle and the release of myoglobin (protein) into the blood.
TREATMENT OF NEUROMUSCULAR DISEASES
As for treatment, there is no specific therapy. The therapeutic approach is based on creating the prerequisites for successful rehabilitation and providing high quality general and specialized care.
- Drug therapy. The goal is to compensate for the energy deficiency of muscle tissue, improve tissue metabolism and peripheral circulation. Myotropic drugs and anabolic steroids are used. In the case of Duchenne muscular dystrophy, glucocorticosteroids are used. In the case of myasthenia gravis, anticholinesterase drugs are used. For secondary damage and/or dysfunction of the central nervous system, courses of neuroprotective and neurotrophic therapy are carried out. Drug therapy for bulbar and pseudobulbar disorders.
- Physiotherapy. The goal is to correct metabolic disorders, improve neuromuscular conduction, normalize muscle tone, and prevent the development of contractures.
- Physiotherapy. The goal is to prevent the development and correction of contractures of the limbs, maintain motor activity, improve muscle tone, delay the development of atrophies, and prevent complications caused by inactivity. Teaching the patient how to use assisted sitting and standing devices.
- Orthopedic correction.
- Early detection of swallowing disorders (dysphagia) and the possibility of drug correction (together with ENT doctors, based on the results of nasopharyngoscopy - the functional state of the epiglottis, the presence of regurgitation, and in older children + analysis of the results of an X-ray contrast study of the act of swallowing).
- Neurological assessment of respiratory function (ENMG analysis of the phrenic nerves + ultrasound of the diaphragm, analysis of respiratory function, pulse oximetry and capnometry, mechanics and type of breathing, ECHO data, ECG with a cardiologist’s conclusion).
Neurological examination of patients for respiratory failure makes it possible to clarify its causes, reversibility of disorders and the degree of their compensation. In the case of an established dependence on mechanical ventilation, work in a team of doctors to create a multifunctional therapeutic program that is aimed at improving physical condition and restoring normal life functions. choice of treatment methods and their order (medication and non-medication, including management of respiratory support parameters, breathing exercises, physical therapy, physiotherapeutic techniques, psychological assistance, etc.).
Among hereditary diseases affecting the muscular and nervous systems, there is a very large proportion of those forms that can be accompanied by an intellectual defect. In some of these diseases, the intellectual defect is congenital and nonprogressive; in others, it manifests itself very early and progresses slowly. So, hereditary
Neurological and neuromuscular diseases should and do occur in the population of mentally retarded children. Among congenital or early-onset ataxias and paraplegia alone, there are at least 40 gene defects accompanied by mental retardation [Kalmykova L. G., 1976]. However, most of them are very rare; many are described only in single families, often among the descendants of parents who are in a consanguineous marriage.
In our experience, in the contingent of mentally retarded children examined in a medical genetic consultation, the entire group of progressive diseases of the nervous and muscular systems as a whole makes up a small proportion. The most common of them are Duchenne myopathy and myotonic dystrophy. Children suffering from these diseases, before the development of pronounced manifestations from the muscular system, often come under the supervision of a child psychiatrist with a diagnosis of mental retardation.
Myotonic dystrophy
(atrophic myotonia, dystrophic myotonia, Steinert-Button disease). The disease was first described in detail in 1909. Its incidence varies from 1:50,000 to 1:10,000. An unusually high prevalence of myotonic dystrophy (1:3000) was found in Northern Sweden.
Clinical picture. The disease varies very sharply in clinical picture and timing of onset. In a typical picture, it begins in the 2nd-4th decade of life and is characterized by the development of the following symptoms: myotonia, muscle atrophy, especially of the face, neck, distal limbs, cataracts, early baldness, gonadal atrophy. However, mental retardation occurs with the prenatal onset of this disease.
The most characteristic symptom of intrauterine damage is pronounced bilateral paresis of the facial muscles, the so-called facial diplegia: the face is amicable, the mouth is open, the patient cannot wrinkle his forehead, close his eyes, or smile. At the same time, parents often notice such a face in their child from the first weeks of life. Children suck very poorly and do not smile. Congenital myotonic dystrophy is also characterized by general muscle hypotonia. The muscles are soft and doughy to the touch. Tendon reflexes are sharply reduced or absent. Breathing due to damage to the respiratory muscles is rapid and superficial. Swallowing is often difficult, the cry is very weak. Congenital deformities are often encountered - clubfoot, hyperostosis and asymmetry of the skull, arthrogryposis; the sky is always sharply narrowed, it is high, arched.
Dystrophic and especially myotonic symptoms, characteristic of the disease with its usual, late onset, in children with the intrauterine form of the disease are detected only at an older (preschool) age, but even then, unlike affected adults, they are weakly expressed. Cataracts (a very common symptom of late onset of the disease) usually do not occur in children.
In older children, atrophic changes in the muscles already appear. One can also note symptoms characteristic of adult patients, such as depressions in the area of the temporal fossae due to muscle atrophy, and mild atrophy of the muscles of the legs. Sometimes there is a peculiar growth of hair on the forehead - bald patches on both sides. Myotonic symptoms in school-age children are sometimes easily identified during clinical examination: children slowly and with difficulty unclench their clenched fingers during repeated action.
Mental retardation at the onset of the disease in utero occurs in all affected people: IQ from 20 to 70 units.
The question of the presence of progression in intellectual decline in children is controversial. There is no true progression at the clinical level. Moreover, some positive dynamics are noted in the development of motor skills and speech. Patients are characterized by severe lethargy and helplessness, even in the absence of noticeable motor disorders. As a rule, they are timid and obedient.
Severe dysarthria due to changes in the facial muscles and tongue muscles is very characteristic. In this case, speech has a pronounced nasal tone due to pharyngeal paresis.
The diagnosis is made based on the clinical picture; it can be finally confirmed in doubtful cases by electromyography, which reveals changes characteristic of myotonia, as well as molecular diagnostics of the mutant gene.
The disease is caused by an autosomal dominant gene with sharply varying expressivity. The mutant gene is almost always transmitted by the mother. Inheritance of the defect from mothers may be associated with severe endocrine disruption in affected men, leading to infertility. The mechanism of action of the mutant gene and the pathogenesis of mental retardation are unclear. But the structure and localization of the mutation have been determined. The disease is caused (similar to Martin-Bell syndrome) by amplification, i.e., an increase in the number of nucleotides in a certain region of one of the chromosomes (19ql3,3). The number of nucleotide repeats increases as the mutation is passed on from generation to generation. The severity of the disease clearly correlates with the number of these repeats. The largest number of them is determined in congenital severe form of the disease. The identified mechanism explains the phenomenon of anticipation - the severity and earlier onset of the disease in descending generations.
Treatment. There is no specific treatment. In the presence of atrophy, anabolic steroids (retabolil, nerobol) and general restorative therapy are used. In cases where there are significantly pronounced myotonic symptoms, courses of diphenine are prescribed at 0.03-0.05 g 3 times a day, lasting 2-3 weeks. It is assumed that diphenin has an inhibitory effect on synaptic conduction and reduces post-tetanic activity in muscles [Gecht B. M., Ilyina N. A., 1982].
Prenatal diagnosis of carriage of the myotonic dystrophy gene is currently available.
Progressive muscular dystrophy
(Duchenne myopathy) as an independent clinical form in the group of muscular dystrophies has been quite well studied. It was first described in detail in 1868. The frequency in the population is 1:30,000.
Clinical picture. It is observed almost exclusively in boys. The main symptomatology of the disease is a progressive increase in dystrophic changes with gradual immobilization of the patient.
The lower extremities are primarily affected. The first symptoms appear, as a rule, at the age of 2-4 years, although before this, already in the 1st-2nd year of life, the motor activity of patients is usually reduced. Children begin to walk later, do not run, do not climb onto chairs, etc. Later, a specific (“duck”) gait develops, waddling from side to side.
Pseudohypertrophy of the calf muscles is characteristic with an increase in diffuse muscle atrophy. The calf muscles become dense and increase in volume. Tendon reflexes disappear, but in the early stages of the disease they may even be slightly increased.
The process has an ascending nature: in addition to the legs, muscle weakness spreads to the muscles of the back, chest, and upper limbs. By the age of 13-15, patients are usually completely immobilized. Death occurs at the end of the 2nd decade most often from acute heart failure or pneumonia.
According to various authors, 30-70% of patients with Duchenne myopathy suffer from mental retardation. The latter precedes the appearance of muscle disorders and does not increase, despite the progression of the disease itself.
The degree of intellectual underdevelopment may vary. Patients with a mild decrease in intelligence predominate, but there are cases of mental retardation in the degree of imbecility.
Diagnosis. The congenital nature of the intellectual defect in combination with symptoms of myopathy, manifested in the early stages mainly by a delay in the development of motor skills, often causes diagnostic errors when examining a child at an early age. In these cases, residual effects of organic brain damage with mental retardation and the atonic form of childhood cerebral paralysis
The differential diagnosis should take into account the nature of muscle disorders: more severe damage to the proximal parts of the muscles of the extremities compared to the distal ones, very pronounced muscle hypotonia. In doubtful cases, the diagnosis is clarified using electromyography. The ECG shows changes characteristic of muscle damage.
Progressive Duchenne muscular dystrophy is caused by a recessive gene located on the X chromosome.
The pathogenesis of mental retardation in this disease is not completely clear. Anatomical changes in the brain, as a rule, are not detected, although in some cases changes in cortical cytoarchitecture with neuronal heterotopia are described.
Treatment. There is no effective pathogenetic therapy. General strengthening treatment is carried out, including biogenic stimulants, autohemotherapy, and vitamins.
Drugs that improve protein synthesis are used in the treatment of patients, in particular anabolic hormones (Nerobol, Retabolil). A positive effect was observed from the use of allopurinol, an inhibitor of xanthine oxidase involved in the breakdown of purines, as well as drugs from the group of adrenergic blockers.
When deciding on the prognosis of offspring in women with established carriage of the Duchenne myopathy gene, the method of choice is to determine the sex of the fetus.
Make an appointment with a doctor
To sign up for a cycle, choose any method:
- call the clinic +7 (495) 103-99-55,
- order a call back,
- leave a request for an appointment using a convenient form on the website:
SIGN UP
At the Kuntsevo Medical and Rehabilitation Center, we have created all the conditions so that you can undergo rehabilitation from 8 am to 10 pm on weekdays and from 9 am to 9 pm on weekends.
Our center is within walking distance from the Molodezhnaya metro station.
If you are driving, a nice addition will be free parking for our visitors.
Rhabdomyolysis
With muscle injuries (more common in athletes), gradual destruction of tissue occurs, this condition is called rhabdomyolysis. This process ultimately ends with the death (necrosis) of cells and the release of toxins into the circulatory system. This disease can cause serious complications and lead to kidney failure. If qualified assistance is not provided, it can result in death.
Possible reasons:
1. Bodily injuries (injuries, beatings, accidents, accidents).
2. Stage 3 and 4 burns.
3. Long surgical operations (more than 8–10 hours).
4. Long-term compression of tissues with impaired blood supply.
5. Electric shocks.
The development can be provoked by: increased loads during training, epileptic seizures, severe muscle spasms, delirium tremens.
It is very difficult to recognize the disease; the manifestations are similar to the symptoms of many diseases; sometimes rhabdomyolysis occurs secretly. Often the correct diagnosis can only be made based on the results of a blood test. In an advanced form, the patient may fall into a coma and die.